Dr. Rodolfo Gordigiani
Gynaecological Surgery in Florence
LAPAROSCOPY
ISTEROSCOPIAOPERATIVE COLPOSCOPY
COLPOSCOPIACustomised gynaecological surgery
Surgical Specialities Procedures
Dr. Rodolfo Gordigiani and his team of expert gynaecological surgeons offer a wide range of specialist procedures to address various gynaecological conditions.
These procedures include ovary removal, tubal ligation, and other interventions involving the uterus.
With a focus on individualised treatment and attention to overall patient well-being, we are committed to providing high-quality surgical care that meets your specific needs.
LAPAROSCOPY
Laparoscopy is a surgical technique used by Dr. Rodolfo Gordigiani that deserves special mention. It is a minimally invasive procedure that allows the surgeon to access the abdominal and pelvic cavities through significantly smaller incisions compared to traditional surgery.
This approach offers numerous advantages, including reduced cosmetic damage and faster postoperative recovery. Laparoscopy is used in various situations, such as the treatment of persistent pelvic pain or infertility. Additionally, it is useful for the diagnosis and treatment of conditions such as endometriosis, benign uterine tumours (fibroids), ovarian cysts, and uterine tumours. If you would like further information or wish to book a consultation, please feel free to contact us.
What is laparoscopy?
The laparoscopic procedure involves making a small number of incisions, positioned above the pubic area and laterally to it. Through these incisions, the doctor inserts a laparoscope and the necessary instruments to perform the intervention. The laparoscope is a tool equipped with a network of optical fibres at the end, which serves as both a light source and lenses connected to an external camera.
The Advantages of Laparoscopy
Some advantages of laparoscopy compared to traditional surgery include:
- Shorter hospitalisation
- Less post-operative pain and blood loss
- Less noticeable scars
Dr. Gordigiani also uses this procedure therapeutically, for example, for: Hysterectomy
- Removal of uterine fibroids/myomas
- Removal of one or both ovaries
- Removal of one or both fallopian tubes
- Removal of ovarian cysts of any type
Laparoscopy represents a significant advancement in modern surgery, allowing for effective treatments with less impact on the body.
Description of the Laparoscopic Operation
The surgical procedure is performed under spinal anaesthesia and only in specific cases under general anaesthesia, with oro-tracheal intubation. Thin surgical instruments and a laparoscope (camera) are inserted into the abdomen through micro-incisions ranging from 5 to 15 mm in diameter. During the procedure, the abdominal cavity is distended using a gas mixture of CO2, which is rapidly absorbed at the end of the operation. The duration of the procedure varies depending on the anatomical region involved. As standard practice for all surgical procedures, a venous access is established to administer necessary medications. Additionally, a urinary catheter is inserted after sedation, which is usually removed shortly after awakening unless there are specific clinical needs to retain it. At the end of the procedure, it may be necessary to place an abdominal drain and/or a nasogastric tube, which are removed in the following days. For some procedures involving the urinary tract, it may be necessary to place a ureteral stent (mono or bilateral), an internal device that keeps the ureter open and is not visible externally. The timing of stent removal also varies based on clinical needs.
Blood/plasma transfusions are extremely rare. However, the operating facility is equipped with a Postoperative Intensive Care Unit, with anaesthesiology and nursing staff dedicated 24 hours a day. Restoration of normal feeding in the postoperative period depends on the physiological restoration of intestinal activity and is generally early, unless procedures directly involving the intestinal loops require a slightly longer time frame.
Where clinically feasible, early mobilisation is encouraged to promote a faster postoperative recovery. Typically, hospitalisation, from admission to discharge, lasts on average 48-72 hours, but may extend up to 7 days or more for more complex interventions (such as those involving the intestines, urinary tract, or bladder).
It is common to experience mild discomfort at the site of skin incisions, but this is generally short-lived and can be managed with common analgesics. Additionally, tenderness in the clavicular area, related to irritation of the phrenic nerve, is also frequent and temporary.
In the postoperative period, the patient may experience paresthesias or hypoesthesias of the skin, subjective sensations of mild alteration of skin sensitivity (such as "numbness", tingling, or warmth), especially in the abdominal area or lower limbs (inner thigh). These effects are generally due to the position assumed during the procedure and tend to resolve spontaneously in most cases within a few days, although in rare cases they may persist for a few weeks."
Indications for Laparoscopy
Infertility
When a patient desires pregnancy but encounters difficulty conceiving, laparoscopy can help the doctor identify and sometimes correct the involved pathology. Through the use of an endoscope, the surgeon can check whether the fallopian tubes (through which the fertilised egg passes) are patent or not. In particular, the presence of pelvic endometriosis or adhesions cannot be evaluated with other methods. The fimbria, which is the most distal portion of the tube and serves for the capture of the ovum, can be correctly highlighted only through laparoscopy.
During the laparoscopic examination, in addition to visualising the pelvic organs involved in reproductive function (uterus, tubes, ovary, peritoneum), some procedures are performed routinely, while others only if necessary.
In particular, chromosalpingoscopy is always performed. It consists of injecting, through the cervical canal and via the vaginal route, a vital dye (methylene blue). The filling of the tubes and the passage through the fimbriae into the peritoneum are observed. This test verifies tubal patency.
In extreme cases, in women already candidates for assisted reproductive techniques (IVF/ICSI), in which the pathology has irreversibly compromised tubal function, there is an absolute indication for removal of one or both tubes (salpingectomy).
Adnexal Pathologies
Laparoscopy can be used for conservative or demolitive treatments concerning adnexal pathologies:
Conservative treatment:
• Ovarian biopsy
• Ovarian drilling
• Enucleation of ovarian or tubal cysts
• Enucleation of paraovarian or paratubaric cysts
• Conservative removal of ectopic pregnancy
• Removal of ovarian fibroids
• Lysis of periovarian or peritubal adhesions
• Treatment of hydrosalpinx or PID
• Drainage or removal of tubo-ovarian abscess
Demolitive treatment
• Ovariectomy
• Salpingectomy
• Salpingectomy for ectopic pregnancy
• Adnexectomy
Endometriosis: A Surgical Perspective
• Endometriosis represents one of the best indications for surgical laparoscopy. This technique can successfully treat cases of endometriosis of varying severity, including endometriotic cysts or large nodules.
• Endometriosis is an enigmatic disease that affects millions of women of reproductive age (3-10%) worldwide. Although rare before menarche, it tends to decrease significantly after menopause.
• The term "endometriosis" derives from the word "endometrium," which is the tissue lining the inner surface of the uterus. During the menstrual cycle, the endometrium grows and then sheds.
• In endometriosis, endometrial tissue, histologically identical to that of the endometrium, is located outside the uterus in other parts of the body. These lesions can take the form of cysts, nodules, lesions, implants, or growths. The most common sites include the pelvis, involving ovaries, tubes, uterine ligaments, the area between the vagina and rectum, the outer surface of the uterus, and the lining tissue of the abdominal cavity (peritoneum). Sometimes, these lesions are also found in post-surgical abdominal scars, on the small intestine or rectosigmoid, near the ureters, on the bladder, in the vagina, on the cervix, and on the vulva.
• Similarly to the lining of the uterus, endometriotic lesions are generally responsive to menstrual cycle hormones. Each month, they develop, shed, and cause bleeding. However, in these cases, the endometrial tissue cannot exit the body, resulting in internal bleeding. This leads to changes in blood and shed tissue from the lesions, inflammation of the surrounding areas, and scar tissue formation.
Complications and Symptoms of Endometriosis
Endometriosis can lead to various complications, including:
1. Rupture of lesions: This can cause the spread of endometriosis to other areas.
2. Formation of adhesions: These can cause pain and limit the functionality of the involved organs.
3. Bleeding: Endometriotic lesions can bleed, causing further inflammation and pain.
4. Intestinal obstruction: If endometriosis is located in the intestines, it can cause obstruction.
5. Urinary disorders: Endometriosis near the ureter or bladder can affect urination.
The most common symptoms of endometriosis include:
• Dysmenorrhea: Pain before and during menstruation.
• Dyspareunia: Pain during sexual intercourse.
• Dyschezia: Pain during defecation.
• Diarrhoea and/or constipation.
• Dysuria: Painful urination.
• Chronic pelvic pain.
• Haematochezia/rectorrhagia: Bleeding in stools.
• Hematuria: Blood in urine.
• Nausea/vomiting.
• Menstrual irregularities.
Some women with endometriosis may be asymptomatic, but infertility affects about 30-40% of women with this condition. The intensity of pain is not always correlated with the size of the lesions. Prostaglandins, substances involved in inflammatory processes, often contribute to the symptoms of endometriosis. The staging of the disease is performed during surgery and includes four stages according to the classification of the American Fertility Society (rAFS).
Stages of Endometriosis and Myomectomy
Endometriosis presents in different stages, each with specific characteristics:
1. Stage I (minimal disease): Isolated endometriotic foci are observed, adhering to the outside of the uterine wall, tubes, and ovaries.
2. Stage II (mild disease): There is not always a correlation between the extent of symptoms and the severity of endometriosis. Even a few endometriotic foci can cause severe pain.
3. Stage III (moderate disease): Blood-filled cysts can form in the ovaries. These cysts, when incised during surgery, release a viscous mass of brownish color, hence the name "chocolate cysts." In this phase, adhesions and endometriotic nodules may be present.
4. Stage IV (severe disease): In this stage, cyclical bleeding of the endometriotic focus causes continuous irritation of the peritoneum. This leads to the formation of scars (adhesions) and endometriotic nodules that can penetrate into organs and adjacent structures, such as the intestine, bladder, ureters, and vagina. In severe cases, there is often involvement of the recto-vaginal septum. However, marked endometriosis may not cause any pain.
Uterine Fibroids: A fibroid is a benign mass of fibro-muscular tissue that can develop on the outer surface or inside the uterus.
Myomectomy: Myomectomy, the removal of one or more fibroids, is a conservative surgical intervention aimed at restoring the anatomical and functional integrity of the uterus. During myomectomy, fibroids are removed, allowing for a better quality of life for patients.
The removal of uterine fibroids, also known as myomas or fibromyomatous nodules, is done by peeling off the capsule that clearly delineates them from the surrounding tissue. This capsule often allows for easy removal. To remove fibroids from the abdominal cavity, a specific instrument called a "morcellator" is used, which grinds the fibroids and allows for their removal through small skin incisions. In some cases, the intervention requires a larger skin incision, but for large nodules, a higher incision may be necessary, positioned a few centimeters above the navel.
The size, number, and position of fibroids can influence the difficulty of the intervention. Myomectomy, which preserves the uterus, is preferable to hysterectomy (complete removal of the uterus) in young women, allowing for the possibility of future pregnancy.
The intervention can be performed in two main ways:
1. Laparotomic Myomectomy: with an incision on the abdomen, used for large or numerous fibroids.
2. Laparoscopic Myomectomy: with 3 small incisions of about 5 mm on the abdomen, preferable for small-sized neoplasms.
The postoperative course varies depending on the technique used and the patient's subjectivity, but it is important to avoid excessive efforts in the weeks following the operation.
Laparoscopic Hysterectomy and Pelvic Adhesions
• Laparoscopic hysterectomy is a surgical procedure that allows for the complete removal of the uterus, and if necessary, also of the ovaries and fallopian tubes. This procedure is performed through four small incisions in the abdomen, reducing postoperative pain, accelerating recovery, and improving aesthetic appearance.
• During laparoscopic hysterectomy, a specially designed uterine manipulator is used. This instrument has larger dimensions and a series of silicone valves to ensure the disconnection of the uterus without losing gas pressure inside the abdomen, which would otherwise escape through the vagina. Once laparoscopically disconnected, the uterus is removed vaginally, and the vaginal vault is closed with continuous sutures. In some cases, the procedure may require a larger incision, positioned a few centimeters above the navel.
• Hysterectomy may be associated with other procedures, such as repair of pelvic floor defects (such as cystocele, urethrocele, and rectocele) or prevention of vaginal vault prolapse. These interventions are performed to address disorders related to pelvic structure. In cases of large uteri, the incision may be higher, but always carefully planned to ensure the best outcome.
• Pelvic Adhesions: Peritoneal adhesions are one of the main causes of painful abdominal subocclusive and occlusive syndromes. These conditions often require multiple surgical interventions and can have a significant impact on morbidity and mortality. The increase in patients with adhesive syndrome is correlated with the increase in average life expectancy and survival after abdominal surgery for neoplasms. Laparoscopic techniques have revolutionized the treatment of adhesions, offering positive outcomes and reducing the risk of new adhesion formation.
Adhesion Syndrome and Laparoscopy: A Clinical Perspective
• The increase in patients with adhesive syndrome is correlated with the increase in average life expectancy and survival after abdominal surgery for abdominal tumors. In the past, symptomatic adhesive syndrome was treated through laparotomy (traditional abdominal incision). However, this procedure could trigger the pathophysiological mechanism responsible for adhesion formation. Fortunately, the spread of laparoscopic techniques has revolutionized the treatment of adhesions, offering positive outcomes and reducing the risk of new adhesion formation.
• The laparoscopic approach allows for direct visualization inside the peritoneal cavity, both for diagnostic and therapeutic purposes. This technique improves the patient's quality of life and offers excellent outcomes.
• Sometimes, to assess the presence of adhesions, it may be necessary to make an incision into the abdomen two fingers below the left costal arch along its median line (Palmer's Point). Subsequently, the presence of adhesions below the umbilicus is checked, and only under visual control, the optical trocar is inserted.
Pelvic Floor Defects and Treatments
• Involuntary loss of urine (incontinence) is a personal and social problem. To diagnose stress incontinence, the patient is asked to cough several times with a full bladder. This form of incontinence, called stress incontinence, should be distinguished from urge incontinence, which is caused by overactivity of the detrusor muscle of the bladder. Urge incontinence is more common in elderly women and may benefit from pharmacological and behavioral treatments.
• Stress incontinence, especially if associated with pelvic organ prolapse, often requires surgical treatment. Until a few years ago, the classic procedure for stress incontinence was anterior colporrhaphy (plastic). However, this technique has a low long-term success rate. Other methods have been proposed, including the Burch colposuspension. This relatively simple procedure, which does not require hysterectomy, offers long-lasting results.
• Burch colposuspension can also correct the vesico-urethral prolapse associated with urinary incontinence. Mixed forms of urinary incontinence (stress incontinence associated with urge incontinence) require a case-by-case study to determine the most effective and safe therapy.
• The sling procedure vaginally, also known as T.V.T. (Tension-free Trans-Vaginal Tape) or T.O.T. (Trans-Obturator Tape), is a minimally invasive surgical procedure used to treat stress urinary incontinence in women. In this technique, a synthetic sling is placed around the urethra to ensure continence during activities such as coughing or running.
• Laparoscopic promontofixation is another intervention aimed at correcting uterine prolapse or vaginal vault prolapse. In this procedure, the vaginal vault is suspended and fixed to the uterosacral ligaments.
• Laparoscopic McCall colposuspension is another surgical technique used to correct vaginal prolapse. This involves suspending the vaginal vault on the uterosacral ligaments and obliterating the Douglas pouch.
• Finally, laparoscopic repair of lateral cystocele defects (paravaginal repair) and laparoscopic repair of rectocele are procedures that address specific problems of vaginal prolapse and are performed through the laparoscopic approach.
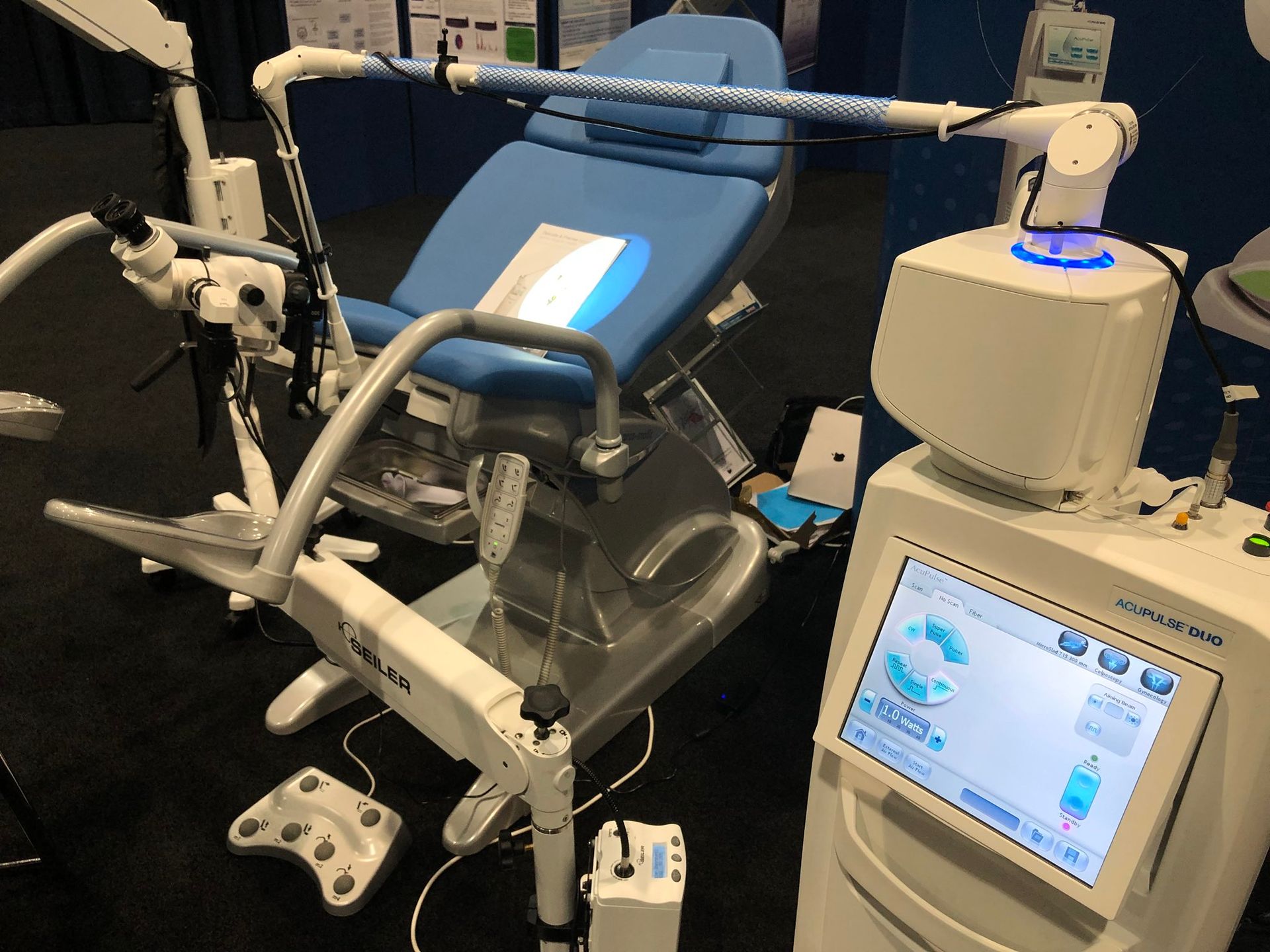
COLPOSCOPIC-GUIDED LASER SURGERY
The growing interest in the use of CO2 lasers spurred research into accessory instrumentation until the coupling of the laser's articulated arm with a microscope or colposcope was devised.
The laser beam control system was achieved through the use of a micromanipulator. It consists of a metal ring and a mirror reflecting the laser beam, manoeuvrable via a joystick. This system allows the laser beam to be directed under direct colposcopic control. Additionally, the beam can be more or less focused, depending on the surgeon's needs, through a mechanical system located at the articulation of the articulated arm.
Such a system can be adapted to any type of colposcope or microscope. The use of the more or less focused laser beam has paved the way for a new type of minimally invasive surgery that has allowed, over time, all interventions on lower genital tract pathologies to become outpatient procedures with or without the use of local anaesthetics.
The main pathologies treated:
The main pathologies in which the technique of operative colposcopy is employed are:
• Conisations
• Remodelling of the External Urethral Orifice (OUE) in cases of cervical infertility
• Vestibulectomy
• Resection of vaginal septa
• Drainage and cauterisation of vaginal cysts
• Excision of suspicious lesions in the vulvar area
• Widening of the vaginal orifice in cases of strictures (post-inflammatory or post-partum)
• Treatment of Bartholin's gland cysts
• Treatment of condylomas in any district of the lower genital tract
• Removal of hamartomas at any level, both vulvar and inguinal.
Consultation and Booking
If you'd like to learn more about our laser treatments, surgical procedures, or vaginal plastic surgeries, don't hesitate to get in touch with us to book a consultation with Dr. Rodolfo Gordigiani.
We're here to answer your questions, discuss your treatment options, and create a personalized plan that suits your needs.
Take the first step towards better gynecological health today.
VAT No. 07253710482